Colonic Diverticular Disease
Vladimir Bolshinsky MD
Scott R. Steele, MD, MBA
Published: November 2018
Expire: November 2021
Definition
A diverticulum is an abnormal pouch arising from an opening within the wall of the alimentary tract.1 The presence of acquired diverticula in the colon is known as colonic diverticular disease. Asymptomatic diverticular disease may be referred to as diverticulosis. Symptoms of diverticular disease include hemorrhage, inflammation (diverticulitis), stricture or obstruction, and fistulae.
Incidence and Epidemiology
The incidence of diverticulosis in the Western world has progressively increased over the past century. Diverticular disease results in nearly 130,000 hospitalizations in the United States each year and more than 1.5 million outpatient visits.2-4 The incidence of diverticular disease is evenly distributed in males and females but increases with age occurring in less than 10% of those younger than 40 compared with up to 70% of those 80 and older.5 However, more recent data demonstrate an increase in the rate of admissions in patients aged 18 to 44 years who are more likely to be male and have more aggressive disease.6-7 The majority of patients with diverticular disease remain asymptomatic with 25% developing symptoms in their lifetime.8
In the West, diverticulosis is predominantly left sided, with 65% of patients with disease limited to the sigmoid colon, 7% of patients with pan colonic disease, and 4% of patients with isolated disease proximal to the sigmoid.9 In Asian populations, 13% to 25% of patients have primarily right colonic diverticulosis.10
Risk Factors
The risk for diverticular disease in influenced by genetic, environmental, and epidemiologic factors (Table 1).
Table 1. Factors Involved in the Pathogenesis of Colonic Diverticulosis
Genetic factors
|
Environmental factors
|
Epidemiologic factors
|
Diet
It has been postulated that a diet rich in dietary fiber reduces from the development of colonic diverticulosis, while a diet heavy in processed meats with a paucity of fiber may explain the prevalence of diverticulosis in industrialized countries. The total intake of dietary fiber was found to be inversely proportional to symptomatic diverticular disease,11 and African and Japanese immigrants who adopted a Western diet developed diverticular disease at a similar rates to their adopted countrymen.12
The etiology of how high levels of red meat and fat consumption contribute to the development of diverticulosis is poorly understood, though endoscopic studies found diets rich in red meat and lipids are associated with an increased risk of diverticular disease13 and studies of diet found vegetarian patients have a lower risk of hospitalization compared with individuals who consume meat.14
The belief that ingestion of undigested foods such as nuts, seeds and popcorn can precipitate complications of diverticular disease by lodging in colonic diverticula is inaccurate. Patients should be advised to follow a healthy diet and eat all foods in moderation. A recent prospective trial demonstrated an inverse relationship between the risk of diverticulosis or diverticular complications and consumption of nuts and popcorn. Consumption of popcorn twice a week may be protective against the disease.15
Alcohol, caffeine, smoking and medications
There is no evidence about the effect of alcohol and caffeine on the development of diverticulosis so there are no recommendations regarding consumption of alcohol and caffeine. Though the data are limited, cigarette smoking is associated with adverse effects related to diverticular disease, rate of hospitalization, and the incidence of perforation.16
Diverticular bleeding and inflammation has been associated with aspirin and nonsteroidal anti-inflammatories drugs while statins appear to have protective qualities.17,18 A threefold increased risk of perforation was reported in patients taking steroids at the time of symptoms and a 70% increased risk in patients with a history of steroid use.18 High dose Vitamin D has been associated with a reduced risk of inflammation.19
Body weight and exercise
Increased body mass index, waist circumference, and hip to waist ratio have been associated with an increased risk of diverticulitis and diverticular bleeding.20 Furthermore, body habitus may be prohibitive of certain operative interventions. Physical exercise is known to have a protective effect on the development of symptomatic diverticular disease.21
Genetic predisposition
Ehlers-Danlos, Marfan syndrome, and polycystic kidney disease have been associated with development of diverticular disease.22,23 Data exploring these associations are limited though it seems intuitive that genetic conditions that may influence the integrity of connective tissues would predispose to diverticulosis.
Pathophysiology
Formation of Colonic Diverticulae
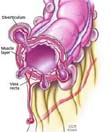
Colonic diverticulae are acquired outpouchings of mucosa and muscularis mucosa that develop on the mesenteric side of the colonic wall (Figure 1). The colon has multiple layers; an internal mucosal layer, an inner circular and an outer longitudinal muscle layer, and a serosal covering. Acquired diverticulae do not contain a muscular or serosal layer and therefore are thin walled. The longitudinal muscle forms 3 distinct tinea coli. Small appendices epiploicae are attached along the side of the colon and share the same blood supply as the mucosa. It must be noted that the longitudinal muscle layer fans out to encompass the rectum, which is also absent of appendices epiploicae. The rectum is spared of diverticular disease.
Diverticulae develop where the circular muscle layer is penetrated by vasa recta to supply the mucosa, a point of weakness in the colonic wall.24 This defect is enlarged by increased intraluminal pressure and is thought to be related to constipation and consequent straining to evacuate. The high colonic pressures can contribute to muscle hypertrophy. The sigmoid colon is the narrowest segment of the large bowel, another theoretical precipitant of segmental diverticulosis.
Asymptomatic diverticulae are typically soft and reducible. They are frequently found incidentally on colonoscopy and abdominal computed tomography (CT) scans. The majority of patients with diverticulosis are asymptomatic. While the incidence of diverticulosis is high, the incidence of diverticulitis is low with less than a quarter of patients progressing to have symptoms over a lifetime.3
Development of Diverticulitis
The progression of diverticulosis to diverticulitis is poorly understood. The traditional belief is that fecal stasis and obstruction of a diverticulum leads to ischemia, ulceration, bacterial overgrowth and micro perforation. This can lead to peri-diverticular or pelvic abscess, as well as free perforation. The first attack of diverticulitis is commonly the most aggressive with patients being most likely to develop free perforation. Follow-up attacks are less likely to require emergent surgery, as the site of inflammation is more likely to be have been walled off by adhesions of omentum, or other viscera.
Development of Diverticular Bleeding
Diverticular bleeding is thought to be associated with baropressure causing the vasorecta to stretch and rupture. It is arterial bleeding from a branch at the dome or neck of the diverticulum.25 Histological assessment of the bleeding point has demonstrated an absence of diverticulitis.26 As such, this condition is painless and is not associated with colonic inflammation. It must be stressed that rectal bleeding and pain is typically associated with a form of colitis and not diverticular disease. Diverticulosis in such patients is not infrequent, but most likely unrelated.
Diagnostic Evaluation
Clinical Presentation
Acute diverticulitis can be uncomplicated, smoldering, or complicated. The acute presentation is typically described as a constellation of “left sided appendicitis” characterized by left lower quadrant pain, fevers and leukocytosis, which is highly suggestive of sigmoid diverticulitis.27 An astute clinician must be aware of a mobile sigmoid colon that will result in suprapubic or right sided peritoneal signs due to local irritation of the abdominal wall by the inflamed sigmoid colon. Common differential diagnoses of sigmoid diverticulitis are described in Table 2. Routine investigations include blood, serum, and urine analysis as well as radiological imaging. These tests help classify the severity of disease and guide management. Diverticulitis involving other parts of the colon is atypical and is much more difficult to diagnose without focused radiological imaging.
Table 2. Differential Diagnosis for Patients Presenting With Symptoms of Sigmoid Diverticulitis
| Colitis: Infective, inflammatory, ischemic |
| Appendicitis |
| Colon cancer |
| Urogenital pathology |
| Ectopic pregnancy |
| Bowel obstruction |
Smoldering diverticulitis is a condition where patients have persistent symptoms of uncomplicated diverticulitis, but are refractory to medical management while not progressing to diverticular complications. A list of diverticular complications, known as complicated diverticulitis is described in Table 3. Patients with such complications are unlikely to respond to medical therapy alone and require operative intervention.
Table 3. Complications of Diverticulitis
| Intraabdominal Abscess |
| Free perforation and peritonitis |
| Colonic stricture and bowel obstruction |
| Enteric fistula (colovesical, colovaginal, colocutaneous) |
| Small bowel obstruction |
| Ureteric obstruction |
| Diverticular Bleeding (complication of diverticulosis) |
Classification of Disease
Assessment of severity in acute diverticulitis can be time critical. The Hinchey Classification, first published in 1978,28 is the most common method used to grade the severity of acute disease. Currently, the modified Hinchey Classification is more frequently utilized due to the advances in diagnostic and interventional radiology (Table 4).29
Table 4. Modified Hinchey Classification of Acute Colonic Diverticulitis
| Stage 0 | Mild clinical diverticulitis |
| Stage Ia | Confined pericolic inflammatory phlegmon |
| Stage Ib | Confined pericolonic abscess (within sigmoid mesocolon) |
| Stage II | Pelvic, distant intra-abdominal or intraperitoneal abscess |
| Stage III | Generalized purulent peritonitis |
| Stage IV | Fecal peritonitis |
Imaging in Diverticular Disease
Though the diagnosis of diverticulitis can be made on history and physical examination, radiological adjuncts help to gauge acuity and aid with the management plan. There is still a role for an abdominal film in the appropriate settings. This is a quick and readily available investigation that will demonstrate signs of obstruction or pneumoperitoneum, and direct subsequent investigation and intervention.
American Society of Colon and Rectal Surgeons guidelines state that CT imaging is the most appropriate initial imaging modality in the assessment of suspected diverticulitis, while Ultrasound and magnetic resonance imaging can be useful alternatives in patients who have relative contraindications to CT scan (pregnancy, renal insufficiency, contrast allergy).27 Using CT imaging with intravenous and luminal contrast, clinicians are able to diagnose complications of diverticulitis with a sensitivity as high as 98% and specificity of 99%.30 More so, cross sectional imaging provides the ability to diagnose other intra-abdominal pathologies that may mimic diverticulitis.31 Combining rectal contrast with CT cross-sectional imaging increases the accuracy further, with a reported specificity of 100%.32
The use of contrast enema studies is limited in light of CT imaging. In select cases of suspected large bowel obstruction, the dynamic role of a (gastrografin) enema study may increase the rate of contrast reaching the right colon compared with CT.
Endoscopic Evaluation of the Colon
The latest American Society of Colon and Rectal Surgeons guidelines recommend that in the setting of a first episode of diverticulitis, or where recent colonoscopies have not been performed, the colon should be endoscopically evaluated to confirm the diagnosis, following resolution of acute symptoms.27 Typically, an elective colonoscopy is scheduled 6 to 8 weeks following the attack.
In cases of complicated diverticular disease, where a colonic fistula is present, a colonoscopy can confirm the site and etiology of the fistula.
Management of Diverticular Disease
An algorithm for the management of patients with diverticular disease is presented in Table 5. Details as to the reasoning for this algorithm are described below.
Table 5. Algorithm for the Management of Patients With Diverticular Disease
| Disease complexity | Severity | Medical and interventional management | Definitive operative management |
| Uncomplicated | Hinchey 0 (first presentation) |
|
No role for surgical intervention |
| Hinchey 0 (recurrent episode) |
|
Consider elective resection if disease effecting quality of life | |
Hinchey 0 or I
|
|
Elective sigmoid colon resection | |
| Complicated | Hinchey II |
|
Surgical resection if symptoms progress following percutaneous drainage or during evolution of diverticular complications |
| Hinchey III |
|
Surgical resection with consideration of fecal diversion. Laparoscopic washout in selected cases |
|
| Hinchey IV |
|
Surgical resection with fecal diversion | |
| Diverticular stricture |
|
Surgical resection with anastomosis and consideration of proximal diverting ostomy | |
| Acute large bowel obstruction |
|
Surgical resection with likely fecal diversion | |
| Colovesical/ Colovaginal fistula |
|
Surgical resection with consideration of temporary fecal diversion. Removal of fistula tract Repair of bladder and/or vagina |
|
| Diverticular bleeding |
|
Subtotal colectomy and end ileostomy indicated in patients with persistent bleeding not controlled with endoscopic and angiographic interventions. |
CT = Computed tomography; IBD = Inflammatory bowel disease; PRBC = packed red blood cells.
Uncomplicated Acute Diverticulitis
The notion that patients with uncomplicated diverticulitis are able to be managed in the outpatient setting is supported by a consensus from multiple national and international guidelines.33 For patients with mild, Hinchey I diverticulitis, the role of antibiotics is controversial. Recent randomized Dutch and Swedish trials demonstrated that in 6 to 12 months there was no significant difference in time to complete recovery or recurrence rates in either the antibiotic or observation arms.34,35 The latest recommendation for the treatment of uncomplicated acute diverticulitis published by the American Gastroenterological Association institute advises selective administration of antibiotics based on patient characteristics.36
Acute Diverticulitis With Abscess
Patients presenting with Hinchey II diverticulitis with an abscess ≥ 4 cm typically require percutaneous drainage, while patients with smaller abscesses typically respond to antibiotics alone.37,38 Percutaneous drainage is frequently performed via a trans-abdominal approach. For pelvic abscesses not amendable to drainage via the abdominal wall, a trans-gluteal approach is considered, though this is typically associated with greater patient discomfort. Transrectal or transvaginal drainage may be performed in select patients.
Patients who are not amendable to percutaneous drainage can be safely treated with antibiotics alone.39 This may be a good option as a bridge to surgery in patients who can benefit from preoperative optimization.
Acute Diverticulitis With Peritonitis
It is not possible to clinically differentiate between Hinchey III and Hinchey IV generalized peritonitis. This diagnosis is made intraoperatively. Feculent peritonitis (Hinchey IV) develops in the setting of a ruptured diverticulum and free perforation. Purulent peritonitis (Hinchey III) is due to a ruptured diverticular abscess, in which case the original perforation had time to be sealed. Operative therapy for purulent or feculent peritonitis should generally include a resection of the diverticular segment.27 The extent of resection should include the acutely diseased colon with margins of healthy colon and rectum. The decision to create an anastomosis in the presence of generalized peritonitis is dependent on patient factors and is individualized. Creating a diversion proximal to the inflamed diverticular segment, without resection of the sigmoid colon, was the historical approach to the emergent treatment of perforated diverticulitis, but is now only reserved for the most difficult scenarios.
Laparoscopic lavage has been described as an alternate surgical modality in patients with Hinchey III peritonitis. While an attractive option that avoids the morbidity of colonic resection and possible stoma formation, it is currently not recommended by the American Society of Colon and Rectal Surgeons due to a high failure to obtain source control.27
Diverticular Stricture With Colonic Obstruction
Colonic obstruction due to acute diverticulitis is uncommon. Classically, a stricture develops due to gradual contraction of the colonic wall in the setting of chronic inflammation.
Typically, patients present with symptoms of progressive obstruction due to gradual stricture formation at the site of a previous attack of acute diverticulitis. A diverticular stricture should be managed as a colonic adenocarcinoma until proven otherwise, as such resection with a lymph node clearance is required in such patients.40 Colonic stenting, though of limited benefit, has been described as a bridge to definitive surgery in patients that would benefit from preoperative optimization.41 A prompt completion colonoscopy or virtual colonoscopy is required exclude synchronous colonic pathology.
Diverticular Disease With Associated Fistulae
The rate of fistula formation in the setting of diverticular disease is well recognized and can develop in up to 2% of cases.42 Colovesical fistulas are most common and are responsible for 50% of all fistulas associated with diverticular disease.42 Colocutaneous fistulas typically occur following interventional radiology drainage of a diverticular abscess, where an internal opening persists in the colonic wall. Colovaginal fistulas occur in women with a previous hysterectomy. Coloenteric and colouterine fistulas have been described, but are very infrequent. Neoplasia and Crohn’s disease must always be considered as a differential diagnosis, particularly in less common types of fistulas. Colonoscopy is the gold standard test to address the etiology of the colonic fistula. A cystoscopy or vaginoscopy may be of benefit in selected cases.
Colovaginal fistulas present with vaginal discharge, and colovesical fistulas present with pneumaturia or fecaluria. These symptoms are typically associated with significant distress for the patients and their families. It is uncommon for patients to develop systemic sepsis in association with diverticular fistulas, as such the preoperative investigations can be carried out in an outpatient setting. A one-stage resection of the sigmoid colon and associated fistula is typically carried out as an elective procedure.42
Diverticular Bleeding
Diverticular bleeding occurs in 3% to 5% of patients with colonic diverticular disease.43 The principles in managing patients with diverticular bleeding involves: resuscitation, confirmation of diagnosis, hemostasis and prevention of recurrence. Diverticular bleeding can result in large volume blood loss. As such, appropriate resuscitation, monitored environment, and activation of a massive transfusion protocol may be necessary. Diverticular hemorrhage stops spontaneously in up to 80% of patients, with a rebleed rate between 22% to 38%.43
Diagnosis of diverticular bleeding can be confirmed with either colonoscopic or radiological visualization.44 The advantage of colonoscopy is that it is accurate at confirming the etiology of bleeding, localizing the site, and has the potential to control the hemorrhage with endoscopic intervention. The disadvantage of colonoscopy is that without bowel preparation, there is a low cecal intubation rate (55% to 70%),43 as well as up to a 2.5% perforation risk in cases where therapeutic coagulation is utilized.44
Computed tomography angiography (CTA) has superseded the nuclear red blood cell scan and can identify lower gastrointestinal bleeding at rates as low as 0.3 mL/min,43 however the intermittent nature of diverticular bleeding can make the diagnosis challenging. Following radiological identification of diverticular bleeding, selective embolization is successful in 85% of patients.45
Surgery for diverticular bleeding is only indicated in patients who have persistent bleeding not controlled with endoscopic and angiographic interventions.33 Patients without preoperative localization require a subtotal colectomy and end ileostomy. It must be noted that even in patients with preoperative localization, a segmental colectomy carriers a rebleed rate of up to 14%.43
Elective Resections for Recurrent Attacks of Diverticulitis
The notion that an elective sigmoid resection should be performed after a second or third attack of uncomplicated diverticulitis are no longer supported by international guidelines.33 The of elective surgery for patients with a history of diverticulitis should be individualized.27 The surgical risk due to patient specific comorbidities should be balanced against the impact on quality of life due to recurrent attacks.
The rate or recurrence of diverticulitis following a sigmoid colectomy is between 1% and 10%.8 It is thought the reduced bowel luminal diameter of the sigmoid results in a relative high pressure zone, precipitating proximal inflation. Recurrence is reduced by ensuring that all of the sigmoid is resected and the proximal colon is anastomosed to the rectum.46 It must be noted that for patients who have recovered from complicated diverticulitis, an elective colectomy should typically be considered.27
Atypical Presentations of Diverticular Disease
Diverticular disease and colon cancer
The widespread prevalence of diverticular disease and colonic adenocarcinoma in the Western world may sometimes lead to patients presenting with dual pathologies. A causal relationship has been hypothesized, but not proven. These 2 diseases are plausibly separate entities though they share common risk factors: advanced age, obesity, sedentary lifestyle, consumption of increased red meat and lack of dietary fiber. Most recent studies have demonstrated that the risk of colon cancer is not increased in patients after the first year of being diagnosed with diverticular disease.47 The increased incidence of cancer within the first 12 months reflects the difficulties with differential diagnosis and common symptomatology and screening effects.
Diverticular disease in patients younger than 50
Historically, episodes of diverticulitis in young patients were considered to be more aggressive so a lower threshold for operative surgery was advised. Due to cumulative risk, younger patients have a higher rate of recurrence, but this is still relatively low (27%), furthermore, only 7.5% of young patients go on to require subsequent emergency surgery.48 As such, routine elective resection based on young age (< 50 years) is no longer recommended by the American Society of Colon and Rectal Surgeons.27
Diverticular disease in the immunosuppressed
Immunosuppressed patients are more likely to fail medical management of acute diverticulitis. They are more likely to undergo emergency surgery and develop recurrences and complications of acute diverticulitis,33 thus a lower threshold for elective resection following an attack of uncomplicated diverticulitis should be considered in these patients.42 Prophylactic resection in transplant patients with proven diverticulosis remains controversial.27,33
Segmental colitis associated with diverticulosis (SCAD)
SCAD is a colonic inflammatory disorder thought to be within the spectrum of inflammatory bowel disease.49 The same entity has also been called diverticular colitis and diverticular disease-associated colitis. The exact pathophysiology of SCAD is unknown, though it has been postulated that fecal stasis and microbial dysbiosis associated with diverticulosis can act as an environmental trigger to precipitate segmental colitis.50,51 The incidence of SCAD is 4 in 100,000, with a median age of 68, similar to the second peak of inflammatory bowel disease.52
Following endoscopic assessment and histological grading, patients are treated as a mild form of inflammatory bowel disease, typically with mesalamine enemas, local steroids (beclomethasone) and probiotics.49
Summary
- The incidence of diverticular disease, particularly diverticulitis, has increased in industrialized countries.
- Diverticular disease can be classified as uncomplicated disease, uncomplicated recurrent or smoldering disease, and complicated disease.
- The first attack of acute diverticulitis is usually the most severe.
- Conservative or medical management is usually indicated for acute uncomplicated diverticulitis. Surgery is reserved for complicated diverticular disease, and in selected cases of recurrent uncomplicated attacks.
- The aim of surgery is typically to resect the segment of sigmoid colon, as residual sigmoid colon increases the rate of recurrent symptoms.
- Diverticular bleeding is associated with diverticulosis and not diverticulitis.
References
- Merriam-Webster Dictionary. Diverticulum. www.merriam-webster.com/dictionary/diverticulum. Accessed September 28, 2018.
- Munson KD, Hensien MA, Jacob LN, Robinson AM, Liston WA. Diverticulitis: a comprehensive follow-up. Dis Colon Rectum 1996; 39(3):318–322.
- Biondo S, Golda T, Kreisler E, et al. Outpatient versus hospitalization management for uncomplicated diverticulitis: a prospective, multicenter, randomized clinical trial (DIVER Trial). Ann Surg 2014; 259(1):38–44.
- Shaheen NJ, Hansen RA, Morgan DR, et al. The burden of gastrointestinal and liver diseases, 2006. Am J Gastroenterol 2006; 101(9):2128–2138.
- Jacobs DO. Diverticulitis. N Engl J Med 2007; 357(20):2057–2066.
- Etzioni DA, Mack TM, Beart RW Jr, Kaiser AM. Diverticulitis in the United States: 1998–2005— changing patterns of disease and treatment. Ann Surg 2009; 249(2):210–217.
- Lahat A, Menachem Y, Avidan B, et al. Diverticulitis in the young patient—is it different? World J Gastroenterol 2006; 12(18):2932–2935.
- Lin M, Raman SR. Evaluation of quality of life and surgical outcomes for treatment of diverticular disease. Clin Colon Rectal Surg 2018; 31(4):251–257.
- Parks TG. Natural history of diverticular disease of the colon. Clin Gastroenterol 1975; 4(1):53–69.
- Munie ST, Nalamati SPM. Epidemiology and pathophysiology of diverticular disease. Clin Colon Rectal Surg 2018; 31(4):209–213.
- Aldoori WH, Giovannucci EL, Rimm EB, Wing AL, Trichopoulos DV, Willett WC. A prospective study of diet and the risk of symptomatic diverticular disease in men. Am J Clin Nutr 1994; 60(5):757–764.
- Painter NS, Burkitt DP. Diverticular ddisease of the colon: a deficiency disease of Western civilization. Br Med J 1971; 2(5759)450–454.
- Peery AF, Sandler RS, Ahnen DJ, et al. Constipation and a low-fiber diet are not associated with diverticulosis. Clin Gastroenterol Hepatol 2013; 11(12):1622–1627.
- Crowe FL, Appleby PN, Allen NE, Key TJ. Diet and risk of diverticular disease in Oxford cohort of European Prospective Investigation into Cancer and Nutrition (EPIC): prospective study of British vegetarians and non-vegetarians. BMJ 2011; 343:d4131.
- Strate LL, Liu YL, Syngal S, Aldoori WH, Giovannucci EL. Nut, corn, and popcorn consumption and the incidence of diverticular disease. JAMA 2008; 300(8):907–914.
- Böhm SK. Risk factors for diverticulosis, diverticulitis, diverticular perforation, and bleeding: a plea for more subtle history taking. Viszeralmedizin 2015; 31(2):84–94.
- Strate LL, Liu YL, Huang ES, Giovannucci EL, Chan AT. Use of aspirin or nonsteroidal anti-inflammatory drugs increases risk for diverticulitis and diverticular bleeding. Gastroenterology 2011; 140(5):1427–1433.
- Humes DJ, Fleming KM, Spiller RC, West J. Concurrent drug use and the risk of perforated colonic diverticular disease: a population-based case-control study. Gut 2011; 60(2):219–224.
- Maguire LH, Song M, Strate LE, Giovannucci EL, Chan AT. Higher serum levels of vitamin D are associated with a reduced risk of diverticulitis. Clin Gastroenterol Hepatol 2013; 11(12):1631–1635.
- Strate LL, Liu YL, Aldoori WH, Syngal S, Giovannucci EL. Obesity increases the risks of diverticulitis and diverticular bleeding. Gastroenterology 2009; 136(1):115–122.e1.
- Strate LL, Liu YL, Aldoori WH, Giovannucci EL. Physical activity decreases diverticular complications. Am J Gastroenterol 2009; 104(5):1221–1230.
- Leganger J, Søborg MK, Mortensen LQ, Gregersen R, Rosenberg J, Burcharth J. Association between diverticular disease and Ehlers-Danlos syndrome: a 13-year nationwide population-based cohort study. Int J Colorectal Dis 2016; 31(12):1863–1867.
- Lederman ED, McCoy G, Conti DJ, Lee EC. Diverticulitis and polycystic kidney disease. Am Surg 2000; 66(2):200–203.
- Slack WW. The anatomy, pathology, and some clinical features of divericulitis of the colon. Br J Surg 1962; 50:185–190.
- Jensen DM, Machicado GA, Jutabha R, Kovacs TO. Urgent colonoscopy for the diagnosis and treatment of severe diverticular hemorrhage. N Engl J Med 2000; 342(2):78–82.
- Meyers MA, Alonso DR, Baer JW. Pathogenesis of massively bleeding colonic diverticulosis: new observations. AJR Am J Roentgenol 1976; 127(6):901–908.
- Feingold D, Steele SR, Lee S, et al. Practice parameters for the treatment of sigmoid diverticulitis. Dis Colon Rectum 2014; 57(3):284–294.
- Hinchey EJ, Schaal PG, Richards GK. Treatment of perforated diverticular disease of the colon. Adv Surg 1978; 12:85–109.
- Hall J. Diverticular disease. In: Steele SR, Hull TL, Read TE, Saclarides TJ, Senagore AJ, Whitlow CB, eds. The ASCRS Textbook of Colon and Rectal Surgery. 3rd ed. Cham: Springer International Publishing; 2016:645–667.
- Ambrosetti P, Jenny A, Becker C, Terrier TF, Morel P. Acute left colonic diverticulitis—compared performance of computed tomography and water-soluble contrast enema: prospective evaluation of 420 patients. Dis Colon Rectum 2000; 43(10):1363–1367.
- Baker ME. Imaging and interventional techniques in acute left-sided diverticulitis. J Gastrointest Surg 2008; 12(8):1314–1317.
- Rao PM, Rhea JT, Novelline RA, et al. Helical CT with only colonic contrast material for diagnosing diverticulitis: prospective evaluation of 150 patients. AJR Am J Roentgenol 1998; 170(6):1445–1449.
- Galetin T, Galetin A, Vestweber KH, Rink AD. Systematic review and comparison of national and international guidelines on diverticular disease. Int J Colorectal Dis 2018; 33(3):261–272.
- Ünlü Ç, de Korte N, Daniels L, et al; Dutch Diverticular Disease 3D Collaborative Study Group. A multicenter randomized clinical trial investigating the cost-effectiveness of treatment strategies with or without antibiotics for uncomplicated acute diverticulitis (DIABOLO trial). BMC Surg 2010; 10:23.
- Chabok A, Påhlman L, Hjern F, Haapaniemi S, Smedh K; AVOD Study Group. Randomized clinical trial of antibiotics in acute uncomplicated diverticulitis. Br J Surg 2012; 99(4):532–539.
- Stollman N, Smalley W, Hirano I; AGA Institute Clinical Guidelines Committee. American Gastroenterological Association Institute Guideline on the management of acute diverticulitis. Gastroenterology 2015; 149(7):1944–1949.
- Siewert B, Tye G, Kruskal J, et al. Impact of CT-guided drainage in the treatment of diverticular abscesses: size matters. AJR Am J Roentgenol 2006; 186(3):680–686.
- Soumian S, Thomas S, Mohan PP, Khan N, Khan Z, Raju T. Management of Hinchey II diverticulitis. World J Gastroenterol 2008; 14(47):7163–7169.
- Elagili F, Stocchi L, Ozuner G, Kiran RP. Antibiotics alone instead of percutaneous drainage as initial treatment of large diverticular abscess. Tech Coloproctol 2015; 19(2):97–103.
- Venara A, Toqué L, Barbieux J, et al. Sigmoid stricture associated with diverticular disease should be an indication for elective surgery with lymph node clearance. J Visc Surg 2015; 152(4):211–215.
- Tamim WZ, Ghellai A, Counihan TC, Swanson RS, Colby JM, Sweeney WB. Experience with endoluminal colonic wall stents for the management of large bowel obstruction for benign and malignant disease. Arch Surg 2000; 135(4):434–438.
- Neale JA. Surgical management of diverticular disease in the elective setting. Clin Colon Rectal Surg 2018; 31(4):236–242.
- Mohammed Ilyas MI, Szilagy EJ. Management of diverticular bleeding: evaluation, stabilization, intervention, and recurrence of bleeding and indications for resection after control of bleeding. Clin Colon Rectal Surg 2018; 31(4):243–250.
- Pasha SF, Shergill A, Acosta RD, et al; ASGE Standards of Practice Committee. The role of endoscopy in the patient with lower GI bleeding. Gastrointest Endosc 2014; 79(6):875–885.
- Khanna A, Ognibene SJ, Koniaris LG. Embolization as first-line therapy for diverticulosis-related massive lower gastrointestinal bleeding: evidence from a meta-analysis. J Gastrointest Surg 2005; 9(3):343–352.
- Thaler K, Baig MK, Berho M, et al. Determinants of recurrence after sigmoid resection for uncomplicated diverticulitis. Dis Colon Rectum 2003; 46(3):385–388.
- Regula J. Diverticular disease and colorectal cancer: incidental diagnosis or real association? Final answer. J Clin Gastroenterol 2016; 50(suppl 1):S39–S40.
- Eglinton T, Nguyen T, Raniga S, Dixon L, Dobbs B, Frizelle FA. Patterns of recurrence in patients with acute diverticulitis. Br J Surg 2010; 97(6):952–957.
- Kucejko RJ, Poggio JL. Considerations and changes in the evaluation, management, and outcomes in the management of diverticular disease: the diagnosis, pathology, and treatment of diverticular colitis. Clin Colon Rectal Surg 2018; 31(4):221–225.
- Sultan K, Fields S, Panagopoulos G, Korelitz BI. The nature of inflammatory bowel disease in patients with coexistent colonic diverticulosis. J Clin Gastroenterol 2006; 40(4):317–321.
- Ludeman L, Shepherd NA. What is diverticular colitis? Pathology 2002; 34(6):568–572.
- Tursi A, Elisei W, Picchio M. Incidence and prevalence of inflammatory bowel diseases in gastroenterology primary care setting. Eur J Intern Med 2013; 24(8):852–856.